 He is on the Board of Directors for the Intensive Care Foundation and is a First Part Examiner for the College of Intensive Care Medicine. He is also a Clinical Adjunct Associate Professor at Monash University. He is a co-founder of the Australia and New Zealand Clinician Educator Network (ANZCEN) and is the Lead for the ANZCEN Clinician Educator Incubator programme. KI Doc - So much hot gas – ETCO2 for non-anaesthetists (2013)Ĭhris is an Intensivist and ECMO specialist at the Alfred ICU in Melbourne.Should every mechanically ventilated patient be monitored with capnography from intubation to extubation? Respir Care. Respiratory therapies in the critical care setting. See Capnography Waveform Interpretation.Positive pressure ventilation and use of PEEP.Low cardiac output or cardiogenic shock.This usually reflects an increase in alveolar dead space about 5 mmHg is normal (ETCO2 should always be lower than PaCO2) utility in neonates and children may be impaired because of small tidal volumes.analysed circuit gases can also leak to the environment may be inaccurate if low tidal volumes as fresh gas may be entrained (e.g. prone to blocking as not in line with gas flow prediction of PaCO2 from ETCO2 is variable (the major limiting factors = pulmonary blood flow and V/Q mismatch) and ETCO 2 may be misleadingly different in conditions with significant V/Q mismatch.add dead space and weight to the circuit need time to heat up to avoid condensation on the heater cardiac arrest states, a low pulmonary flow due to PE, or large alveolar dead space) false negative results can occur (e.g.stomach contents, adrenaline solution from ampoules) colorimetric CO2 detectors may change colour if exposed to acidic fluid (e.g. high levels of other gases that absorb the infrared light can lead to falsely high readings (e.g. oesophageal intubations after consumption of carbonated beverages or vigorous bag and mask ventilation (although this rapidly ceases after 20–30s or 6-8 ventilations quantitative devices with waveforms reveal a characteristic decrementing, non-square pattern) single beam (sample gas passes through only) or double beam (additional beam with no CO 2 to act as a control) systems.light is focused through the chamber onto a photodetector and the amount detected quantified and converted to a calibrated quantity of CO 2.gas passes through a chamber made of material transparent to infrared light (e.g.Infra-red analysers use spectroscopic sensors to detect CO 2 in a gaseous environment by its characteristic absorption wavelength.test quantitative devices by blowing on them and seeing am ETCO2 trace before placing in the patient circuit.normally ETCO 2 is up to 5 mmHg/0.7kPa lower than PaCO 2 as some alveolar dead space is always present.the detected CO 2 absorbance is converted to a quantitative amount and displayed with a waveform.others are sidestream devices (with aspiration of gas that is transported to a sensor located a variable distance away).some are connected mainstream (flow through via an in-line adapter with universal connectors).can only be used once (colour does not change back, hence only useful for confirmation of ETT position in the trachea during intubation, not ongoing monitoring).devices are inserted on the end of an endotracheal tube or tracheostomy tube and connected to a ventilator circuit (via universal connectors).production of a quantitative ETCO2 value and allows assessment of waveform morphology (ETCO2 vs time).placed in line with ventilation and patient’s airway.Infrared analysers are most commonly used.Capnography provides a display of the quantity of exhaled CO 2 with time which produces a characteristic waveform.  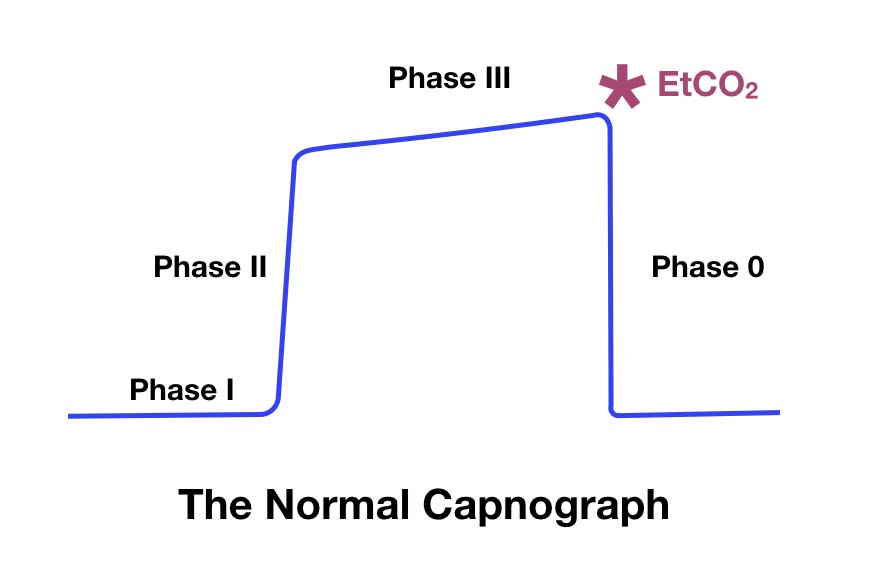
Capnometry devices provides measurement and numeric display of end tidal CO 2 (ETCO 2).detects breath to breath colour changes through a pH detector (metacresol purple on filter paper changes to yellow in the presence of CO 2).sudden decrease -> sudden decrease in pulmonary blood flow -> PE.to provide protection against unexpected hypercapnia in the neurosurgical patient.recognition of spontaneous breath during apnoea testing.assess CPR quality during cardiac arrest (cardiac output) and detect ROSC.allows recognition of different wave forms types which can correspond to various pathologies (e.g.monitoring during mechanical ventilation.via Hudson mask) without mechanical ventilation monitor ventilation during procedural sedation (e.g.To detect and/or measure exhaled CO 2 for 3 main reasons: 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
